Implantable devices that release insulin into the body hold promise as an alternative way to treat diabetes without injections or cannula insertions. However, one obstacle that has prevented their use so far is that the immune system attacks them after implantation, forming a thick layer of scar tissues that blocks insulin release.
Now, a team of MIT engineers and collaborators has devised a device that can prevent scar tissue caused by implantable devices that release insulin to the body.
In a study of mice, they showed that when they incorporated mechanical actuation into a soft device, the device remained functional for much longer than a typical drug-delivery implant. The device is repeatedly inflated and deflated for five minutes every 12 hours, and this mechanical deflection prevents immune cells from accumulating around the device.
For many years, scientists have been working on insulin-delivering devices that could be implanted under the skin. However, the fibrous capsules that form around such devices can lead to device failure within weeks or months.
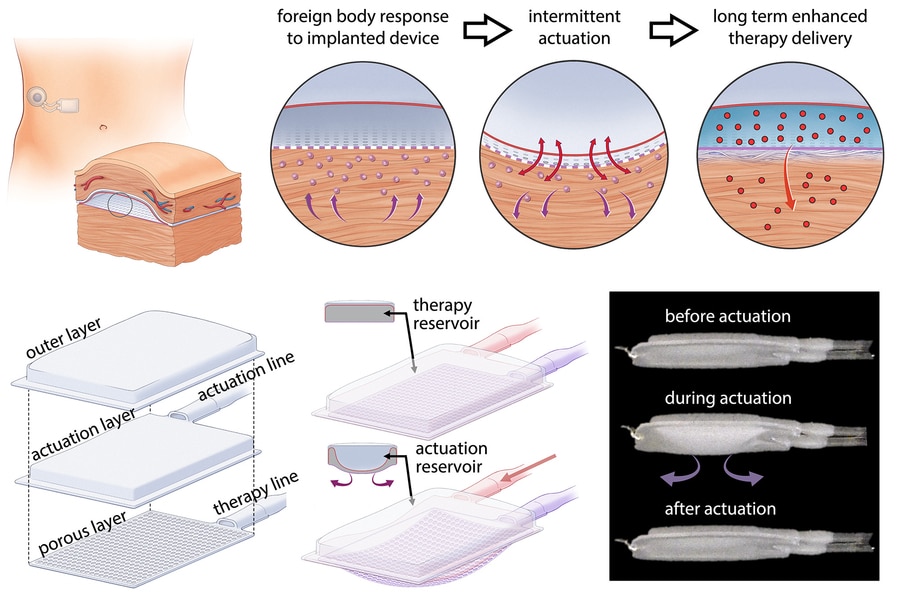
Researchers have tried many approaches to prevent this kind of scar tissue from forming, including local delivery of immunosuppressants. The MIT team took a different approach that does not require any drugs – instead, their implant includes a mechanically actuated device that remained functional for much longer than a typical drug-delivery implant.
In the new study, researchers wanted to see if that immunomodulatory effect could help improve drug delivery. They built a two-chambered device made of polyurethane, a plastic that has similar elasticity to the extracellular matrix that surrounds tissues. One of the chambers acts as a drug reservoir, and the other acts as a soft, inflatable actuator. Using an external controller, the researchers can stimulate the actuator to inflate and deflate on a specific schedule. For this study, they performed the actuation every 12 hours, for five minutes at a time.
“We’re using this type of motion to extend the lifetime and the efficacy of these implanted reservoirs that can deliver drugs like insulin, and we think this platform can be extended beyond this application,” says Ellen Roche, a member of MIT’s Institute for Medical Engineering and Science.
Among other possible applications, the researchers now plan to see if they can use the device to deliver pancreatic islet cells that could act as a “bioartificial pancreas” to help treat diabetes.
The MIT team also created a human-sized version of the device, 120 millimeters by 80 millimeters, and showed that it could be successfully implanted in the abdomen of a human cadaver. “This was a proof of concept to show that there is a minimally invasive surgical technique that could potentially be employed for a larger-scale, human-scale device,” says MIT postdoc Debkalpa Goswami.